Assemble the record
Symptoms, labs, medications, sleep, substances, supplements, and prior treatment response are put in one clinical frame.
The Method
Psychiatric symptoms deserve medical diagnostic reasoning.
Diagnostic Psychiatry connects symptoms, labs, sleep, medications, screening scores, substances, supplements, and timeline before a case is treated as purely psychiatric or simply treatment resistant.
Definition
It does not replace psychiatry. It makes psychiatric evaluation more medically complete. Some symptoms are primary psychiatric illness. Some are medical illness. Some are both. The method leaves room for all three.
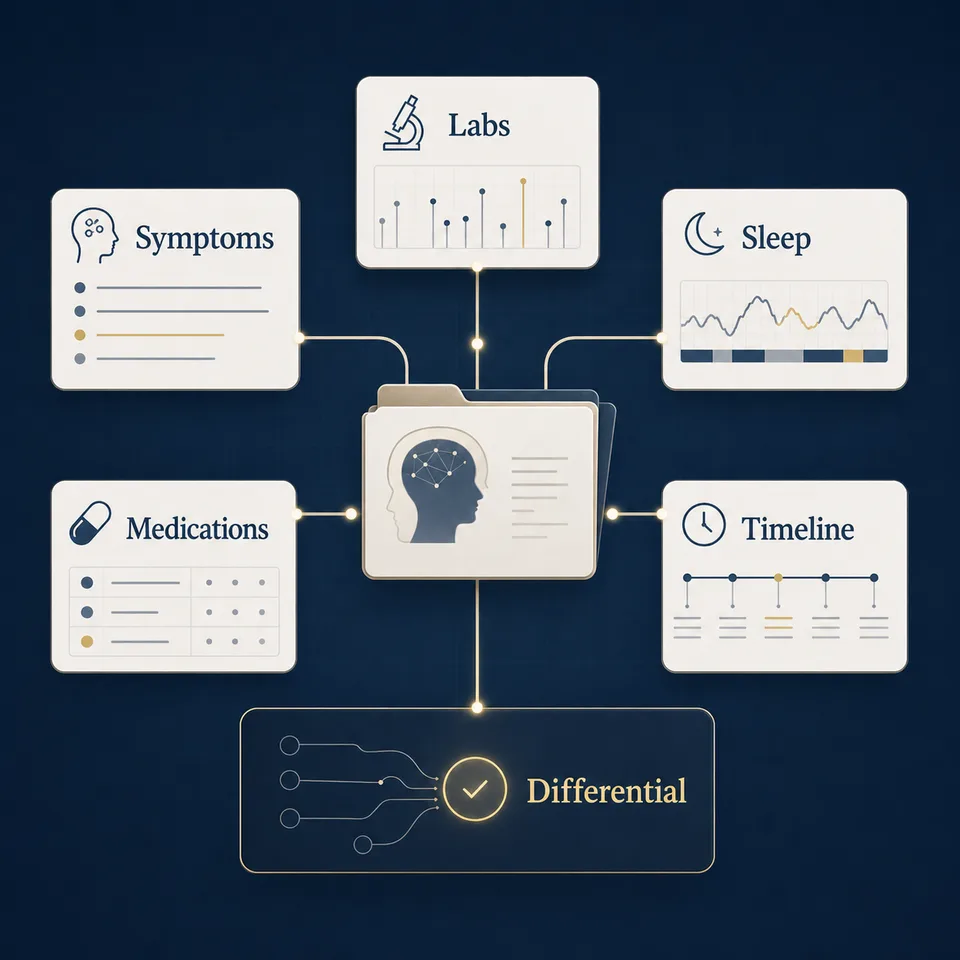
Method frame
Symptoms, labs, sleep, medications, substances, screening scores, and timeline are assembled before interpretation. The output is a differential and a responsible route, not a lab-based identity or a wellness score.
What comes into the review
A red mark changes the question. It does not answer it. Normal range does not always end clinical interpretation. The work is reading the whole pattern.
The review is structured
Symptoms, labs, medications, sleep, substances, supplements, and prior treatment response are put in one clinical frame.
A thyroid marker is read beside panic, weight change, fatigue, sleep, and medication history. A lab is a signal, not a diagnosis.
The review asks what could be psychiatric, medical, sleep-related, medication-related, substance-related, psychological, or mixed.
The output is a clearer pathway: psychiatric care, primary care follow-up, specialist referral, further testing, monitoring, or no medical action.
What the review can change
The goal is not to treat a number. The goal is to understand the person, the pattern, and the next responsible step.
The medical review may support the original psychiatric diagnosis and strengthen the treatment plan.
A sleep, endocrine, nutritional, medication, metabolic, neurologic, or inflammatory pattern may need attention.
Some findings belong with primary care or a medical specialist. The review should say that plainly.
Not every abnormality changes care. Not every symptom needs more testing. That is still a useful result.
Clinical guardrail
Evidence basis
The evidence basis for this framework includes psychiatric evaluation guidelines, major depression treatment guidelines, and review literature on medical and sleep contributors that can mimic or amplify psychiatric symptoms. The page should not be read as a diagnostic or treatment protocol.
Next step
For clinical care, start with the review pathway. For education, continue through the conditions library and method pages.